Tips for Karva Chauth: Traditional Indian Day of Fasting, Love, Celebration & Rejuvenation


Karva Chauth is an ancient tradition practiced by Hindu women especially in Northern India. During this day which involves a fasting ritual, the woman prays for her husband’s good health and long life. It is a day of celebration of love and togetherness, and of gratitude for all the blessings.
After fasting for the entire day, women dress up in colorful traditional clothing and jewelry in the evenings and pray together in a group before sunset, but eating only after sighting the moon in the presence of their husbands in the night.

The visualization of the moon is a big, but fun challenge for all in the household and community. The mischievous moon is most evasive that night!
This day of fasting and prayer incidentally coincides with the change of the season and the cooling of the weather outside. It is an excellent practice as it detoxifies the body as well as the mind, and what better time to do it than at the change of the season.
Biologically speaking, women are practicing intermittent fasting in this tradition. This allows the body, but especially the gastrointestinal system (including the liver) time to rest and release toxic material (Ama, a term for toxins in Ayurveda), and stimulates body organs to rejuvenate and function better. Do remember that during the fast, there is release of a variety of toxins from the body tissues and this can lead to symptoms of aching, fatigue, brain fog, headache and irritability.
It is better to prepare for the day of fasting by starting to clean up your eating habits from a week before the day of the actual fast. This includes giving up alcohol intake and reducing caffeine. Being prepared will result in less adverse symptoms during the actual fasting period.
A few words of caution:
- If you have an illness like cancer, heart disease, kidney disease or a current infection, fasting may or may not be appropriate for you, so always seek medical advice for your unique situation.
- If you are a diabetic, and on either oral medication or insulin for it, please make sure you eat intermittently and/or change your medication schedule on the day of fasting.
- If you are pregnant please do make sure you are consuming fresh fruits and veggies and water or lemonade during the day.
Always consult with you physician whether it is advisable for you to fast at all.
Tips for the morning of the Karvachauth fast:
Traditionally women eat Sargi (a snack) after prayers and before sunrise on the day of the fast. Try to eat protein rich foods, and not eat a high sugar or carbohydrate laden meal. The latter will cause blood sugar fluctuations during the day which will make you more hungry and irritable. Protein, on the other hand, stabilizes mood and blood sugar keeping you full longer.
Nuts are a great option as they not only contain protein but also have excellent essential fats which nurture the brain and body throughout the day.
Make sure to hydrate very well in the morning especially if you follow a strict “no-water” fast!
The fun part:
Remember fasting is not just a ritual for the body, it is also rejuvenation for the mind and our opportunity to return to the wholeness of our souls. It is your time to relax & regenerate! So make the most of it!

A few tips for relaxation & rejuvenation:
- Listen to soothing music,
- Practice meditation or mindfulness,
- Try pranayama (breathing techniques),
- Try restorative yoga techniques or corpse pose (Shavasana) with the intention to heal the body, mind and soul,
- During the day if you have the luxury to be off work (or at least take half a day off!), try to pamper your self with a spa massage or at least do a self-massage (self -abhyanga)
- Don’t over-exert physically or mentally. Read your favorite book.
- If you’re ok with consuming water during the fast, sip some chamomile tea or other herbal teas
- Take a warm bath with a few drops of your favorite essential oils, especially if you feel fatigue, headache, or body aches.
- If nothing else, take a nap or just go see a movie with your friends.
Celebrate YOU!
This is your chance!
Tip on breaking your fast:
After the evening puja (prayer typically done with a gathering of friends), start with a glass or two of room temperature or luke-warm water. You can even add a little lemon, himalayan salt, and honey to the water. Natural, unsweetened coconut water is also a great option for slowly introducing electrolytes back into the body.
I find most women craving for tea or coffee, but those probably are not good ideas as they can cause gastric distress and even nausea.
I would also not recommend consuming any ice cold fluids.

Typically the moon is notorious for playing hide and seek within the clouds on the day of Karva Chauth! Once you’re fortunate enough to having a viewing (hopefully an early one!), follow these tips to introduce food after your fast in a healthy way:
After the moon is out and finally the fast is broken, please venture slowly into eating again.
First add in some fresh fruits in small amounts. Then after a little while have your dinner.
Fresh home made yogurt or coconut kefir (if you are dairy sensitive) are great as they help in the digestion of nutrients which the body greatly needs after a full day of starvation.
Moog lentil soup (daal) with a little white basmati rice and ghee are great options along with some easy to digest well cooked vegetables.
Eating fried and oily foods may be counterproductive as those are harder to digest and our stomach’s digestive fire (agni, an Ayuvedic term) as well as our pancreas may not be ready for such heavy foods.
Finally enjoy and celebrate your time with family and friends!
Many of my patients over the years have asked me to advise them on some tips to fast safely, so I decided to write this blog. Hope you found it useful.
I would love to hear from you about your experiences and any other tips you may have…
Please share and reach me through my social media or email me through my website.
Image source: http://www.4to40.com/greetings/cards.asp?festivals=Karva_Chauth-Karwa_Chauth-163
websol November 20th, 2015
Tags: celebration, detox, detoxification, Fasting, Food, Hindu, India, Indian, Intermittent fasting, Karva Chauth, love, rejuvenation, tradition
A Functional Medicine Physician’s approach to an Overburdened Detoxification System

 You must have heard that “we are what we eat”, but are we really just that? Actually “we are what we eat (or drink), breathe, breakdown, digest, absorb (from our gut and skin), and cannot eliminate from our body, whether it’s through our thoughts, skin, breath, urine and stool! Even though we are designed to have built-in detoxification and elimination pathways, they can get overwhelmed with years of toxin exposures which our bodies are now having to handle more so than ever before in our evolution history.
You must have heard that “we are what we eat”, but are we really just that? Actually “we are what we eat (or drink), breathe, breakdown, digest, absorb (from our gut and skin), and cannot eliminate from our body, whether it’s through our thoughts, skin, breath, urine and stool! Even though we are designed to have built-in detoxification and elimination pathways, they can get overwhelmed with years of toxin exposures which our bodies are now having to handle more so than ever before in our evolution history.Below is a quick check list that I keep in my mind of patients who might have signs of an overburdened detox system.
While the list below is by no means exhaustive, some general evaluation guidelines are:
1. Detailed history and intake with the help of Medical Symptom Questionnaires, Toxicity and Exposure questionnaires, Environmental and Occupational Exposure Questionnaires.
2. Detailed Nutritional, Dental and Physical examination.
3. Conventional Lab tests: can be done from local labs like Labcorp/ Quest etc
Complete Blood Count looking for low white cell count, anemia, low patelet count.
Complete Metabolic Panel looking at liver enzymes, bilirubin levels, alkaline phosphatase, gamma glutamyl transferase levels.
Kidney Function Tests: Blood urea nitrogen, creatinine, cystatin C
Metabolic testing: Fasting and 2 hour post prandial insulin and blood sugar testing, fructosamine, hemoglobin A1C, detailed lipoprotein profile to assess for LDL and HDL particle numbers and sizes and other markers of inflammation specific to the vascular system
Indices like C-reactive protein, ferritin, fibrinogen to evaluate presence of inflammation.
Detailed thyroid function tests along with evaluation of antibodies against thyroid gland.
Iron absorption and storage assessment
4. Functional Labs to test for Biomarkers: These can be:
Stool Assessments: to look for growth of disease causing bacteria/yeast in the gut, and also to assess the balance of good vs bad bacteria in the gut; looking for parasites; markers of inflammation of the gut; markers of deficient detoxifications ability in the gut itself (which can lead to recirculation within our body of our own estrogens, cancer promoters and hormone mimickers from the environment, instead of them being eliminated in the stool); assessment of pancreatic enzymes production; looking for markers of healthy absorption vs malabsorption.
Assessment for nutritional deficiencies (of all fat and water soluble vitamins, minerals, essential amino acids, antioxidants {including the master antioxidant, glutathione}, essential fatty acids). Nutritional support is a key factor influencing the proper functioning of the different phases of detoxification as I have mentioned in my previous blog
Serum testing for food sensitivities (IgG), and environmental and food allergies (IgE).
Specialized genetic and antibody testing for Gluten as well as cross-reactive foods antibodies.
Saliva testing for male and female hormones and adrenal health. If you are placed on Bio-identical hormones, you must periodically also get testeded to see how the hormones are metabolized in your body, which can vary widely. If not adequately metabolized and detoxified these can increase the risk of cancer (like breast, prostate and other hormonally related cancers) development.
Testing for neurotransmitter levels, as well as balance/imbalance between the excitatory and inhibitory neurotransmitters. This can be helpful in patients with anxiety, depression, attention problems or chronic sleep issues.
Looking for heavy metal toxic burden on the body, if indicated by a detailed clinical evaluation. One example of this would be if you have silver mercury amalgam(s) in your teeth especially old ones.
Assessment for signs of oxidative stress or damage (similar to rusting of iron that occurs in nature on exposure to oxygen) to the body due to toxins: these tests look for markers of DNA damage, as well as damage to circulating fats (lipids) in the blood. Damage (aka oxidation) to LDL, the bad cholesterol, may lead to coronary artery disease.
If indicated, checking for chronic stealth infections due to bacteria, parasites and viruses which may harm the immune system and other organ systems. These could present as chronic fatigue, muscle and joint pains, autoimmune diseases and many other vague nagging symptoms.
If indicated, evaluating and testing for mold exposure and mycotoxins. You may need to find a physician who has experience in diagnosing and treating mold related illnesses.
Genomics Testing: to assess for genetic variations known as SNPs (Single Nucleotide Polymorphisms) – like the commonly known MTHFR variants among so many others – which may lead to an increased genetic susceptibility towards accumulating toxins and limit the detoxification capacity of our phase 1 and/or phase 2 liver enzymes.
Most of the above testing can be ordered by any physician, but the interpretation (which really is the key!) can probably only be done accurately by a trained Functional Medicine (FM) Practitioner. I strongly feel that someone with a chronic health issue, should start with a FM doctor as soon as possible, while fully realizing that in some parts of the country and many parts of the world this is not an option. Also, there are some FM practitioners who are not medical doctors and may not be able to order some of these tests. In those cases the tests could be ordered by your regular MD, with results being preferably interpreted by your trained FM Practitioner.
For some general guidelines on how to reduce and manage toxins in your life, you can read my blog..
If you feel that toxicity may be responsible for your chronic health problems, I encourage you to locate an Institute for Functional Medicine Certified Practitioner (IFMCP) in your area and get evaluated.
Good luck in your journey towards optimal emotional, mental and physical health!
websol October 20th, 2015
Posted In: Blog Post, Functional Medicine
12 Tips To Help You Prevent Breast Cancer


During 2017, a whopping 252,7100 new cases of invasive breast cancer are expected to be diagnosed among women in the US; about 2,470 new cases are expected in men (yes, men!). Breast cancer is related to a state of excess estrogens, known as estrogen dominance. Uterine fibroids, breast cysts, PMS, infertility, migraines, and even prostate cancer in men can be related to estrogen dominance.
We really are what we eat, drink, breathe, think, and cannot eliminate! While food most certainly is to be regarded as the best medicine, it can also be the biggest poison. When there’s diminished elimination of physical and emotional toxins, they build up, which may lead to DNA damage and ultimately cancer.
Some of the best strategies for breast cancer prevention are:
1. Food is always first!
Eat antioxidant-rich foods like organic fruits, vegetables, nuts and seeds, and healthy fats and oils like avocado and extra virgin olive oil. Eat your rainbow of 8-10 servings of vegetables and fruits every day to get optimal phytonutrient benefit. Especially include cruciferous vegetables like broccoli, cauliflower, brussels sprouts, kale, cabbage, and bok choy, which provide indole-3-carbinol (I3C), a phytonutrient which helps metabolize estrogen.
Remember: Sugar is cancer’s best buddy! It activates cancer genes and fuels growth of cancer cells. Eliminate sugar from your diet in every shape or form.
2. Quit smoking.
A study published in early 2013 in the Journal of the National Cancer Institute showed that smokers have a 24% higher risk and former smokers have a 13% higher risk of invasive breast cancer than non-smokers.
3. Avoid alcohol.
Alcohol changes the way estrogen is metabolized in our body, which can lead to estrogen dominance. Women who drink alcohol have higher body estrogen levels than those who don’t.
4. Consume a diet low in animal-based foods.
Animal-based products are extremely inflammatory and expose the body to a high dose of arachidonic acid, an inflammatory mediator. Fill half your plate with veggies!
5. Exercise regularly and develop a yoga practice.
Any amount of exercise, mild or intense, will reduce the risk of breast cancer. Aerobic exercise reduce the risk of breast cancer development, by changing the metabolism of estrogen in our body and increasing the ratio of “good” (2-hydroxyestrone) to the “bad” (16alpha-hydroxyestrone) estrogens.
Yoga balances and regulates the endocrine system, and thus our hormones. It also builds the immune system, while promoting lymph flow, the latter being extremely important for drainage of toxins from the breast and the lymph nodes in the axilla (arm pit).
6. Do regular breast self-exams and breast massage.
They can be life saving! Get clinical breast exams at your yearly physicals, and mammograms if appropriate.
7. Maintain the right body composition and fat percentage of your body.
Obesity and visceral adipose tissue (VAT, i.e., the fat accumulated around your abdominal organs) are extremely inflammatory! Find a Functional Medicine practitioner who is trained in First Line Therapy/ Therapeutic Lifestyle Change, a special program specifically targeted to reduce this fat factory of our body.
8. Reduce other inflammation-causing issues in your body.
It’s important to get tested for food sensitivities and eliminate from your diet all foods to which you may have allergies or sensitivities. Get checked for, and treat chronic infections in the gut, mouth and sinuses.
Remember, inflammation makes the immune system less effective in doing its job, and a less effective immune system leads to progression of cancer cells!
9. Avoid toxins.
These can take the form of:
- Inflammatory foods that are filled with trans fats, artificial coloring and preservatives.
- Household cleaning chemicals, pesticides and insecticides.
- BPA-containing plastics, which can be used for storing food and water.
- Personal care products and perfumes: these may contain hormone-disrupting chemicals like pthalates and parabens.
10. Consume a good-quality protein at each meal.
Your body needs essential amino acids at every step to function optimally. Work with your physician to get a comprehensive stool analysis, which will tell you whether the protein you’re eating is getting digested and absorbed as effectively as it should.
11. Balance mind, body and emotions with meditation, breath control and emotional freedom exercises.
Here are a few tips:
- Meditate daily.
- Learn and practice yogic breathing exercises.
- Practice forgiveness every day!
- Journal before going to bed to detoxify the mind.
12. Sleep is your best friend!
A study published in August 2012 showed an association between less sleep and development of aggressive forms of breast cancers in women.
If you suffer from chronic sleep issues, work with your physician to find the underlying cause and correct it. Using drugs isn’t the answer!
I hope to have given you a message of empowerment that you can do something to prevent breast cancer. I would love to hear from you if you’ve used any of these measures.
You can look for a Functional Medicine practitioner in your area here.
This blog first appeared in MindBodyGreen
websol July 20th, 2015
Posted In: Blog Post
15 Simple Ways To Reduce Toxins In Your Life


Every day, we’re exposed to toxins, from our food, water and air! Our body therefore, has a built in, efficient detoxification system which works 24/7, through our liver, gut, skin, kidneys and lungs.
The liver, our main filtration system, has two detoxification phases, and each is very important. The Phase 1 pathway leads to the production of toxic intermediates (free radicals), which then must be rapidly acted upon by the Phase 2 pathway so as to render these harmless. If Phase 1 is overactive and Phase 2 is sluggish for any reason, we run a risk of build-up of the toxic intermediate products from the Phase 1 pathway. These intermediary chemicals are more detrimental than the original toxin itself!
Some simple strategies to reduce your toxic exposure:
1. Stop eating canned food (even if it’s organic)!
Cans are lined with BPA (Bisphenol A), a Persistent Organic Pollutant (POP). POPs can linger in the human body for up to 100 years! POPs preferentially induce Phase 1 enzymes (Cytochrome P450 enzymes) of your liver detoxification pathways, causing production of free radicals, which in turn deplete the antioxidant reserves of your body.
2. Avoid plastic water bottles.
Drink water all day long, but don’t drink it out of plastic bottles! These also contain BPA.
3. Read your make-up ingredients carefully!
Most makeup products (even the brand name ones) contain phthalates and Triclosan, which are endocrine disruptors and hormone mimickers. Your makeup should contain only natural ingredients. Remember, if you can’t eat it, don’t apply it on your skin or body!
4. Use only natural household cleaners!
Synthetic cleaning chemicals produce a byproduct called dioxin, an endocrine disruptor, immune modulator, and carcinogen which induces Cyp1B1, an enzyme of the Phase 1 liver detoxification pathway. This leads to increased production of 4 Hydroxy Estrogen, a “bad” estrogen, associated with breast cancer development.
5. Find a biological dentist and get any silver-mercury fillings, removed safely!
Mercury accumulation in the body can cause autoimmune and neurological problems. It binds to sulfhydryl groups in Glutathione (GSH), the master anti-oxidant of the body, rendering it ineffective in its job as a free radical quencher. Mercury depletes GSH and selenium, a crucial mineral for thyroid health and proper production of thyroid hormones.
6. Stop eating toxic, denatured, pesticide-laden, genetically modified and processed “dead” foods!
Consume grapefruit, onions, garlic, cruciferous veggies, cilantro, parsley, all of which help the liver in its detoxification role. Eat organic whenever you can. Consume a good quality protein at each meal as both the detoxification phases need amino acids to function optimally. Avoid charbroiled meats, which selectively induce phase 1 enzyme, Cyt1A1. If you have concerns about your diet not being optimal in nutrients for any reason, at least consider consuming a good quality multi-vitamin multi-mineral supplement. I’m partial to this brand. (Full disclosure, it’s my line of supplements!)
7. Stop any form of substance abuse.
This includes tobacco, alcohol, drugs, even stimulants like caffeine!
8. Know that pharmaceutical drugs can be the biggest burden for your body to attempt to detoxify.
Always discuss with your physician in detail regarding the need your prescription medications. Review safer options, and understand their side effect profile well.
9. Drastically reduce your stress levels.
Stress is a toxin, especially when chronic! Our body cannot differentiate between emotional and physical stress, and reacts similarly to both, by producing generous amounts of the stress hormone cortisol. When elevated for long periods of time, cortisol can lead to undesirable chronic diseases and symptoms like high blood pressure, weight gain, metabolic syndrome, diabetes, IBS, sleep issues, and it even increases your risk for heart attacks and strokes.
10. Investigate any food allergies.
Food allergies and poor gut health are inflammatory! Excess inflammatory markers chronically circulating in the blood behave like toxins and slow down the efficacy of the liver detoxification mechanisms. A Comprehensive Stool Analysis and a food sensitivity test can help you identify your trigger foods.
11. Lose excess fat.
Fat stores toxins! Lose excess body fat, especially the inflammatory Visceral Adipose Tissue (VAT). Our body’s intelligence believes that the solution to pollution is dilution, and since most toxins are fat soluble, it tries to dilute the blood content of these by pushing them into the fat cells!
It’s crucial to remember that fat reduction should always be done under supervision of a trained health care practitioner. If liver detoxification pathways are not supported before initiating a fat or weight loss program, one can become very sick when fat loss causes release of large amounts of stored toxins into the blood stream. You may have heard of people getting quite ill after losing weight rapidly. So, please exercise caution!
12. Shake it up!
Movement mobilizes toxins! Exercise regularly to gently release toxins through skin via sweat. Yoga is great to enhance lymphatic drainage. Slow deep breathing releases toxins through lungs.
13. Get those bowels moving.
Our gut has been called the “Phase 3” Detoxification pathway! Avoid constipation, so that once the liver has done its job of converting the fat soluble toxins into water soluble compounds, they are easily and rapidly eliminated in the stool. Constipation leads to recirculation of toxins in the body, increasing toxic exposure, thus increasing risk for cancers and other chronic diseases.
14. Prevent emotional toxins from building up!
Practice journaling, meditation, forgiveness, mindfulness, and emotional release techniques on a regular basis. Don’t hesitate to seek professional help if needed.
15. Last, but probably one of the most important is sleep!
It’s the best way to rejuvenate the body’s detoxification capacity both on a mental and physical level. Assess whether you wake up refreshed every morning. If not, please get evaluated for why that is so! It could be the most important thing you did for yourself!
Hopefully some of these simple reminders will help you. For additional individualized help and functional testing of your gastro-intestinal tract health, food sensitivities, toxin testing; adrenal health evaluation, or testing for micro-nutrient, vitamin, mineral and antioxidant deficiencies (which impact your liver’s ability to eliminate toxins), find a Functional Medicine Physician in your area.
websol December 19th, 2013
Posted In: Blog Post
Calming the Vata winds of the holiday season!
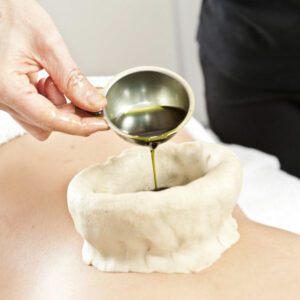

The festive season of fall and winter is a time of reflection on the year gone by and a time to be thankful for one’s blessings. It is also a time of overindulgence in seasonal treats, which compromises the body. To counteract these effects, traditional cultures of the world have devised some simple lifestyle techniques that I use in my Integrative Medicine practice.
Integrative Medicine is the coalescence of modern Allopathic medicine with an upcoming field of medicine called Functional Medicine and traditional and complementary healing methods like Ayurveda. Traditional Chinese Medicine, Acupuncture, Mind-Body healing techniques like yoga, meditation, and healing touch, to name a few. These tools in the tool-box of any Integrative Medicine practitioner are pulled out at the appropriate time. Integrative Medicine is truly “whole”ness in medicine. It is as individualized as it gets! While my main area of focus is Functional Medicine (finding out the root cause of illness, i.e. the ‘how’ and ‘why’ of any disease process), I do integrate it with other ancient healing arts, my favorite being Ayurvedic Medicine, which was an integral part of my upbringing in India.
Ayurveda, a 5000-year-old consciousness based healing tradition from India, is made up of two Sanskrit root words, Ayus (life), and Veda (knowledge) — Ayurveda means the knowledge or wisdom of life. Ayurveda’s premise is that we are an inseparable part of the universe, so are most certainly impacted by even the subtlest of changes in our environment.
According to Ayurveda, at the time of conception each one of us is infused with a different proportion of the five great elements (known as “The Panch Mahabhutas”) — Space (Akasha), Air (Vayu), Fire (Tejas), Water (Jal) , and Earth (Prithvi) which contributes to three major mind-body constitutions or body types of Ayurveda (Doshas) namely, Vata (preponderance of space and air), Pitta (preponderance of fire and water), and Kapha (preponderance of water and earth). While detailed discussions of these three Ayurvedic mind-body types and their subtypes is beyond the scope of this article, it is pertinent to state that the objective of any integrative physician should be to understand and evaluate their patient’s unique Dosha and to try and restore it back into balance.
Environmental changes are very closely mirrored by our body systems. During such transition periods it is of utmost importance to give our body as much nourishment as we can, so with minimal effort it continues to maintain harmony of all organ systems. At these times, I would prescribe an individualized regimen of lifestyle, diet, sleep, exercise, and mind-body techniques to match, balance and support my patient’s individual constitution.
Fall and winter is Vata season (November through February). Vata Dosha controls all movement in mind and body, i.e. blood flow, breathing, waste elimination, movement of thoughts, to name a few. It even governs the movement of Pitta and Kapha Doshas, hence Vata is rightly considered the leader of the three. It is imperative to keep Vata in a balanced state at all times since when out of balance, it pushes the other two Doshas out of balance very easily. The qualities of Vata Dosha are: cold, dry, rough, light, windy and irregular, so an increase in these qualities during the Vata season can cause dry, cracking, dull and rough skin; exacerbate worry, anxiety, irritability, spaciness and sleeplessness (insomnia) in some; cause slowing or irregularity of the bowel transit time leading to constipation, gas, bloating and IBS-like symptoms; cause spells of forgetfulness; painful joints and even easy fatigability.
If one is predominantly of Vata constitution, that is, eating mainly a Vata-aggravating diet (cold, raw foods and liquids), living a Vata-aggravating (irregular schedules) lifestyle, or is in the Vata time of life (from 60 years of age on up), the effect of Vata imbalance on skin, mind and all body organs is even stronger. To counter these, Ayurveda suggests some simple but very effective techniques that reduce the chances of forming toxic residues (Ama) and enhance the flow of vital life force energy (Praana) and build the sweet essence of health and vitality (Ojas) within us:
- Abhyanga: Daily full-body self-massage using warming and heavy Dosha specific Ayurvedic essential oils
- Stay warm, keeping the skin, head and ears covered to prevent further drying and loss of moisture;
- Preferentially using natural silk or wool clothing rather than synthetics;
- Using sweet and floral essential oils in your warm bath regularly;
- Diet: Ayurveda recommends cooking with Dosha specific herbs and spices; drinking warm fluids throughout the day; eating fresh, warm and well-cooked foods and avoiding raw and cold foods like salads. Most certainly avoid processed, stale foods including left-overs as they have no life force or Praana left in them.
- Eat largest meal around noon when the digestive fire (Agni) is at its strongest. To pacify Vata, sweet, sour and salty tastes are best eaten at this time. Eat your meals in a peaceful environment.
- If you are expecting some dietary indiscretions in the day, sip ginger tea or eat some sliced ginger a few minutes before your meal.
- Avoid all stimulants: caffeine, nicotine;
- Practice breathing exercises (Pranayama) daily, especially when stressed and anxious;
- Meditate; practice Yoga daily;
- Maintain regular sleep-wake schedule in spite of irregular and demanding holiday schedules. Routine is the key!
- Ensure regular daily bowel elimination to prevent build up of toxins.
- Keep some “me” time in the midst of the chaos.
My aim is to help explore these expansive wonderful fields of Integrative Medicine and Functional Medicine with the intention to empower one with the basic knowledge of how ‘real’ food and a nourishing lifestyle not only prevents illness but creates a positive impact towards leading “whole-istic” lives.
Cheers to a blessed, healthy and safe ‘Vata’ season in this New Year!
websol December 19th, 2013
Posted In: Blog Post
New FDA warning of postop codeine in children


In a breaking news that is creating huge waves, FDA today issued a warning to physicians, caregivers and parents for the use of the narcotic drug codeine in children during the post operative period following Tonsillectomy or Adenoidectomy. This is a drug that is used for pain relief and also to suppress coughing as a part of many prescription cough remedies. We all know how common these two surgeries are in the pediatric age group especially for sleep apnea! It is unfortunate that this warning to limit use of this drug comes only after multiple children have died and considerable morbidity has happened to others. The premise of Functional Medicine is that one size does not fit all and that treatment options have to be individualized for every patient even for the very same medical diagnosis and this new warning today from the FDA is a prime example of that.
Just to give a background: Codeine is normally metabolized in the liver to morphine as a part of its elimination pathway in the body. It has been found that about 7% of the population has genetic variations (which in Functional Medicine we call SNPs or Single Nucleotide Polymorphisms) which cause them to metabolize codeine more rapidly to Morphine. These individuals are known as “ultra-rapid metabolizers”. Some ethnic groups have a higher preponderance of these “ultra-rapid metabolizers”. For example a whopping 29% of North African and Ethiopians and 6% of African Americans, Caucasians and Greeks fall in this category of people who will produce excessive amounts of Morphine from even regularly administered “normal” doses of codeine. Morphine, as many of you may know can cause suppression of breathing (respiratory depression) and even death in high doses.
These startling high percentages of genetic variations have been pretty much ignored in regular medical practice until now. I find this especially concerning in the light of the fact that although there is an FDA approved genetic test (only way to diagnose this!) to diagnose who are the “ultra rapid metabolizers”, but the test is hardly used except in research circles or by functional medicine practitioners like myself.
I would urge you to definitely have a detailed conversation with your child’s health care practitioner before using codeine and closely monitor your child for signs and symptoms of respiratory depression like difficulty waking up, disorientation, labored breathing, blue color around lips and mouth and fingers (cyanosis) to name a few, even if “normal” doses of codeine are being used.
FDA has a MedWatch Program to report any such incidents. I’ll be closely watching out for any updates to report back to you!
In the meanwhile please do consider the fact that not only is codeine metabolized differently by these genetic variations in the enzymes in your liver, many other drugs are as well. So please consider the necessity of the next drug you place in your mouth!
Sources:
1. More Codeine Fatalities After Tonsillectomy in North American Children
Kelly, et al. Pediatrics 2012; 129:5 e1343-e1347
2. www.FDA.gov
Dr. Manisha Ghei is Board Certified in Internal Medicine & in Integrative & Holistic Medicine. She is also a Functional Medicine Physician and a Certified First Line Therapy Physician and a Certified Perfect Health Ayurvedic Lifestyle (Ayurveda, Nutrition, Yoga & Meditation) Teacher. Her intention is always to provide her patients with personalized and individualized care and to find out the underlying causes for their “dis-ease” instead of implementing the band-aid philosophy of giving drugs and suppressing symptoms! She is always willing to look at alternative and complementary methods of treating chronic diseases and trying to integrate them together with modern medicine, in order to develop a unique treatment plan for each of her patients!
websol August 19th, 2012
Posted In: Blog Post
“Integrative Medicine……Oh, you mean Alternative Medicine”!

Whenever I mention that I am an Integrative Medicine physician, I am asked the question, “what is that”? The next statement usually is, “you mean you practice Alternative Medicine” or “is that Holistic Medicine”? So, I thought that I should begin this exciting journey with my new blog on….. What exactly is Integrative Medicine?
Integrative Medicine, as the name suggests, is an integration of modern Allopathic medicine with a new and upcoming field of medicine called Functional Medicine and age old traditional and complementary healing methods like Ayurveda, Traditional Chinese Medicine, Acupuncture, Herbology, Energy Medicine and Mind-Body healing techniques like yoga, meditation and healing touch among others. This is truly “whole”ness in medicine.
I am a Board Certified Internal Medicine Physician who after graduating from medical school and residency, started my private practice of Internal Medicine and over years cared for thousands of patients in an out-patient set up as well as in the hospital, which included caring for them in the Intensive Care Unit. Throughout this time, I was constantly plagued by the feeling that something was missing in the way we were treating our patients. I finally realized that, the system of using the paradigm of acute care medicine towards treating chronic conditions was totally flawed and failing. In many instances it led to creation of new problems, due to long term mindless drug therapy, without delving into the real cause for the illness. I had decided that I was not going to be a party to this “band-aid” system of medicine where symptoms were being covered without finding the root cause. Hence, began my journey into the field of Integrative Medicine and Functional Medicine.
I am also board-certified in Integrative and Holistic Medicine and now practice Internal Medicine with an integrative and functional medicine approach. My patient and I are in a healing partnership where I am there to listen to them with empathy, advise and empower them with lifestyle tools, but the patient understands and takes the ultimate responsibility for the impact of his/her lifestyle choices and decisions on their health. As an integrative physician, I am a part of a small but rapidly growing body of medical doctors who are trained to dig deep down and try to find the fundamental causes for the disease process. In my experience most of these are related to poor nutrition and lifestyle choices and so, are reversible. At times, I also find that one individual may be genetically predisposed to getting an illness more than another one. in those cases, I work with the patient at length and attempt to educate them on how food and lifestyle choices can help alter that genetic tendency (i.e. genes are the loaded guns ….. lifestyle pulls the trigger!). Of course, there are circumstances where modern medicine options like drugs and surgical treatment become necessary but my aim is to reduce their use and need as soon as it is possible after the acute event is over.
At my office, we practice lifestyle medicine which is in the real sense, Preventive Medicine. Many chronic ailments like type 2 diabetes, high blood pressure, high cholesterol, obesity, metabolic syndrome, irritable bowel syndrome, polycystic ovarian syndrome, allergies among many others can and have been ‘cured’ with simple, therapeutic lifestyle changes. During the extensive investigation into the cause of an illness, we try to assess our patient’s dietary choices and patterns, nutritional needs, exercise and movement habits, sleep hygiene, stress management abilities and skills, inter-personal relationships, family and community dynamics and support systems and spiritual needs, among other factors. The intention is to heal the mind, the body and the soul! This approach of integrating my Western Internal Medicine training with other scientifically-based treatment modalities which have stood the test of time, has helped my patients recover not only from their ‘dis-ease’ but has given them skills for achieving lifelong health as well as mind and body healing and vibrancy during the natural aging process.
It is my constant attempt in my practice, to give my patients the tools needed to take charge of their health with simple and easy changes and also help them understand the connections between their genes and the environment. My aim, on this blog is to explore with all of you, this expansive wonderful field of Integrative Medicine and the intention is to empower you with the basic knowledge of how ‘real’ food and nourishing lifestyle can not only prevent illness but create a positive impact towards leading “whole-istic” lives. Of course, there will be times when I will blog about something relevant to food, nutrition and health that is interesting in the news and possibly useful to the readers.
In the end I would like to congratulate you, the readers and all my patients who are leading the movement towards a shift in the way medicine will be practiced in the future. You are willing to take your health in your own hands and are demanding more and are showing that status quo in medicine will not work! I would be lying if I claimed that Integrative Medicine does not face challenges every day and I hope to discuss those challenges with you in some of my future posts. It is my vision that it is not far from becoming the standard of care…… a few baby steps at a time in our journey together on this path, and I am confident that this will happen sooner than later!
websol October 19th, 2011
Posted In: Blog Post




